This article is a guest post from Lea Chatham, Editor-in-Chief of Kareo’s Getting Paid blog. She develops educational resources to help small medical practices improve their businesses and to help physicians, staff, and patients understand the intersection of healthcare and technology. Her work has been published in many leading journals including Physicians Practice, Medical Economics, Medical Practice Insider, and the PAHCOM Journal.
As the healthcare industry changes, many physicians are moving away from the traditional fee-for-service (FFS) practice model to reduce billing complexity and manage regulatory challenges. ALSO READ: 3 Trends Shaping the Future of Healthcare Technology Kareo’s recent survey, Practice Model Perspectives 2015, revealed which providers are using FFS vs alternate models and how they differ in structure, staffing, and technology use. As it turns out, these variables have a marked impact on which practice model you use.
The top reasons for switching to a concierge, direct primary care (DPC), or other membership models were:
As the healthcare industry changes, many physicians are moving away from the traditional fee-for-service (FFS) practice model to reduce billing complexity and manage regulatory challenges. ALSO READ: 3 Trends Shaping the Future of Healthcare Technology Kareo’s recent survey, Practice Model Perspectives 2015, revealed which providers are using FFS vs alternate models and how they differ in structure, staffing, and technology use. As it turns out, these variables have a marked impact on which practice model you use.
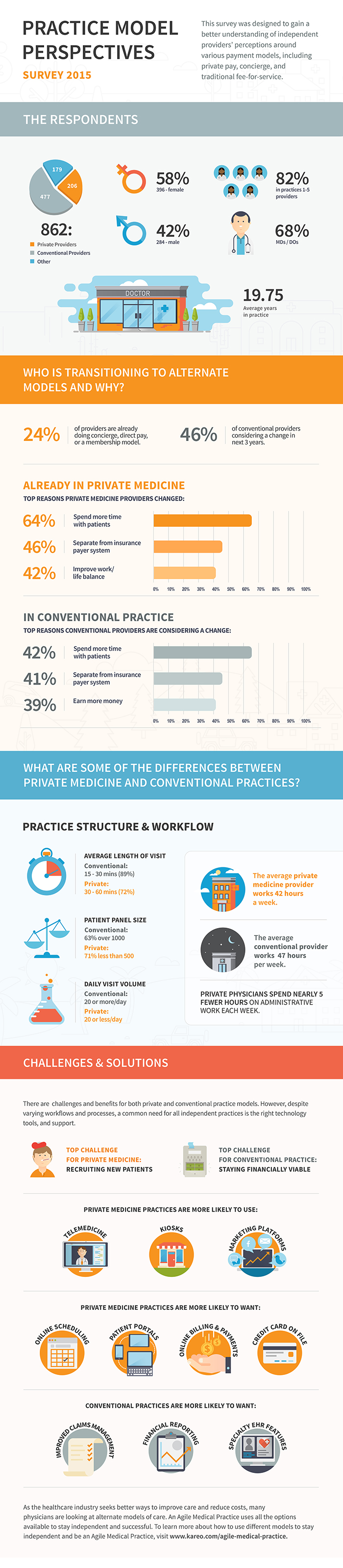 Key Survey Findings
Key Survey Findings
The top reasons for switching to a concierge, direct primary care (DPC), or other membership models were:
- to separate from the insurance payer system, and
- to spend more time with patients.
- Online scheduling (25 percent)
- Online bill payment (20 percent)





